Plantar Fasciosis: Causes, Symptoms & Treatments
 Plantar Fasciosis: Causes, Symptoms & Treatments www.walkjogrun.net
Plantar Fasciosis: Causes, Symptoms & Treatments www.walkjogrun.net 
If you read the title quickly you might assume this article is about Plantar Fasciitis, it’s not. Although the name is obviously quite similar Plantar Fasciosis is a different (albeit related) condition altogether. Both however involve the plantar fascia — a strong and dense connective tissue structure on the sole of your foot that supports the arch of your foot.
Now, before we dig deeper into this topic and discuss symptoms, treatment and other minutiae — we need to clearly state that this is article is not written by a doctor and it’s not meant as any type of a diagnostic tool. What we hope to achieve here is the collecting and presentation of credible information. We want t0 supply it in a simple and straightforward manner that anyone can understand.
What is Plantar Fasciosis?
So, let’s start at the top. What is Plantar Fasciosis? To use one definition: this is the term used to describe the degenerated and non-inflamed phase of plantar fasciopathy (simply heel pain) often caused by the degeneration ( or deterioration) of the plantar fascia. In a certain way Plantar Fasciosis can be thought of as chronic Plantar Fasciitis (sans inflammation), it’s what can happen downstream if you don’t effectively take care of your feet. In sum, it’s chronic stretching, tearing, and degeneration of the fascia at its attachment site (heel). Simple enough right?
What Causes Plantar Fasciosis?
This next logical step is to ask what causes Plantar Fasciosis? The reasons are myriad, and somewhat complex here. The official line is: “recognized causes include shortening or contracture of the calf muscles and plantar fascia”. To try to put that into simple terms… this condition can often be occurring due to repetitive stress or general wear and tear. Risk factors include: sedentary lifestyle, occupations where you are constantly on your feet, the overuse of high heels, or other strenuous activities such as running or dancing. According to some, improper footwear is the number one cause of this malady. Many other conditions can happen concurrently with Plantar Fasciosis, these most often include: obesity and some of the different forms of arthritis.
What are the Symptoms of Plantar Fasciosis?
Now we get to the real fun stuff, what does it actually feel like to have Plantar Fasciosis? The defining characteristic of this condition is not surprisingly heel pain. This tends to be most pronounced when your feet are doing a lot of weight bearing, and it can often occur first thing in the morning or after a period of prolonged rest. The pain will most often be localized right under your heel bone, but it can also manifest itself in a number of other locations throughout the foot.
Other common signs and symptoms of plantar fasciosis include (but are not limited to):
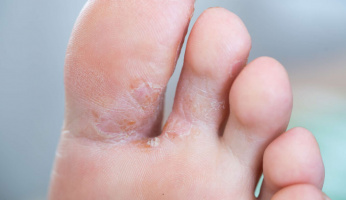
- Mild swelling and redness in your affected area, can sometimes look a bit puffy too
- Tenderness on the bottom of your heel
- Difficult walking and allowing your feet to bear weight in their normal way
- Some people describe burning or stabbing pain along the inside of their foot, especially when walking
How to treat Plantar Fasciosis?
Which brings us to the most important point, what o do about it? Again here is where we would always recommend you defer to professional medical treatment when in doubt. That said, everyone has a slightly different take on the best approach for treating Plantar Fasciosis. We’ve compiled the complete list here for your perusal.
Shoe therapy—finding and utilizing shoes that allow your feet to be in their most natural position— is a great place to start. In some cases this might be the most critical step in addressing plantar fasciosis. Everyone’s feet are different so find what is comfortable for you. But some common thing you want to avoid are heels(obviously), confining toe boxes, and shoes with flat/hard soles.
Some other treatments that doctors often recommend:
- Heat. Given that this is a chronic condition (and not acute like plantar fasciitis), heat (not ice) is the treatment of choice for Plantar Fasciosis. Heat has been shown to help increase blood flow and kick the body’s natural healing mechanisms into gear.
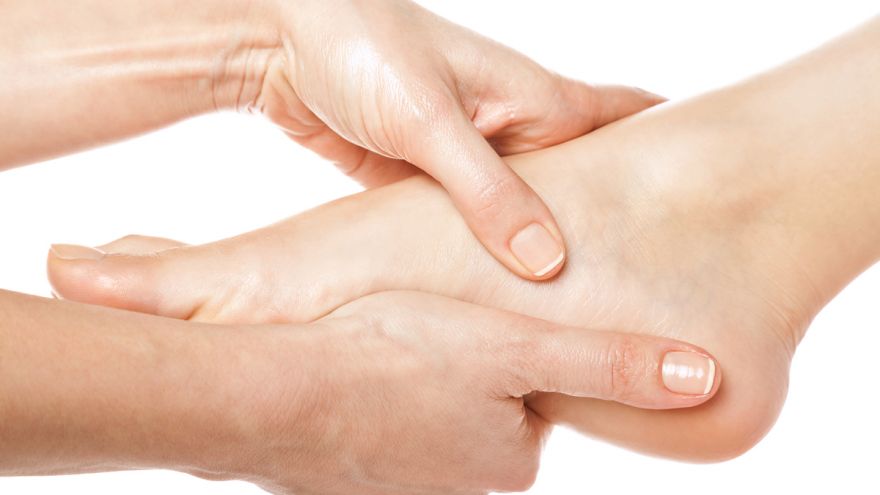
- Massage. Everyone wants an excuse to get a massage, but be cautious here — this is a no go for Plantar Fasciitis but can be a good solution for Fasciosis. Just be clear in what you have and be sure to communicate this to your massage therapist. Massage is another way to try to help your body rebuild some of the degenerated/damaged tissue.
- Foot Exercises. There are some great targeted exercises that can help strengthen and support your feet. Getting a doctor’s recommendation or working with a Physical Therapists in this sense will never hurt. A PT may also be able to help with ultrasound, electrical stimulation, contrast baths, and range-of-motion exercises.
If all of the above doesn’t seem to put a dent in it for you you can always take a more alternative approach and look into acupuncture, reflexology, and magnet therapy. Looking at your diet, or working with a naturalist may be of some benefit as well.
Having pains in your foot or heel is never a good thing. But with appropriate shoes, and a few other preventive measures Plantar Fasciosis can largely be avoided. If you do ever find yourself with intense heel pain that doesn’t seem to go away be cognizant of everything we’ve said above, seek medical attention if needed, and this should ensure you don’t spend too much time away from your favorite activities or job.
Disclaimer
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. The purpose of this website is to promote broad consumer understanding and knowledge. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other qualified health care provider with any questions you may have regarding a medical condition or treatment and before undertaking a new health care regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website.